Explore RCM solutions for DSOs to scale collections, cut AR days, and boost accuracy—without new hires. Real results, fast 7‑day deployment, secure compliance.
Every DSO leader knows the tension: your locations grow, payer rules change weekly, and staffing remains tight. Scaling collections shouldn’t require scaling payroll. This guide lays out a practical path to modern RCM solutions for DSOs—what they are, why they matter now, and how to implement them in under a week while protecting quality and compliance.
What is RCM Solutions for DSOs?
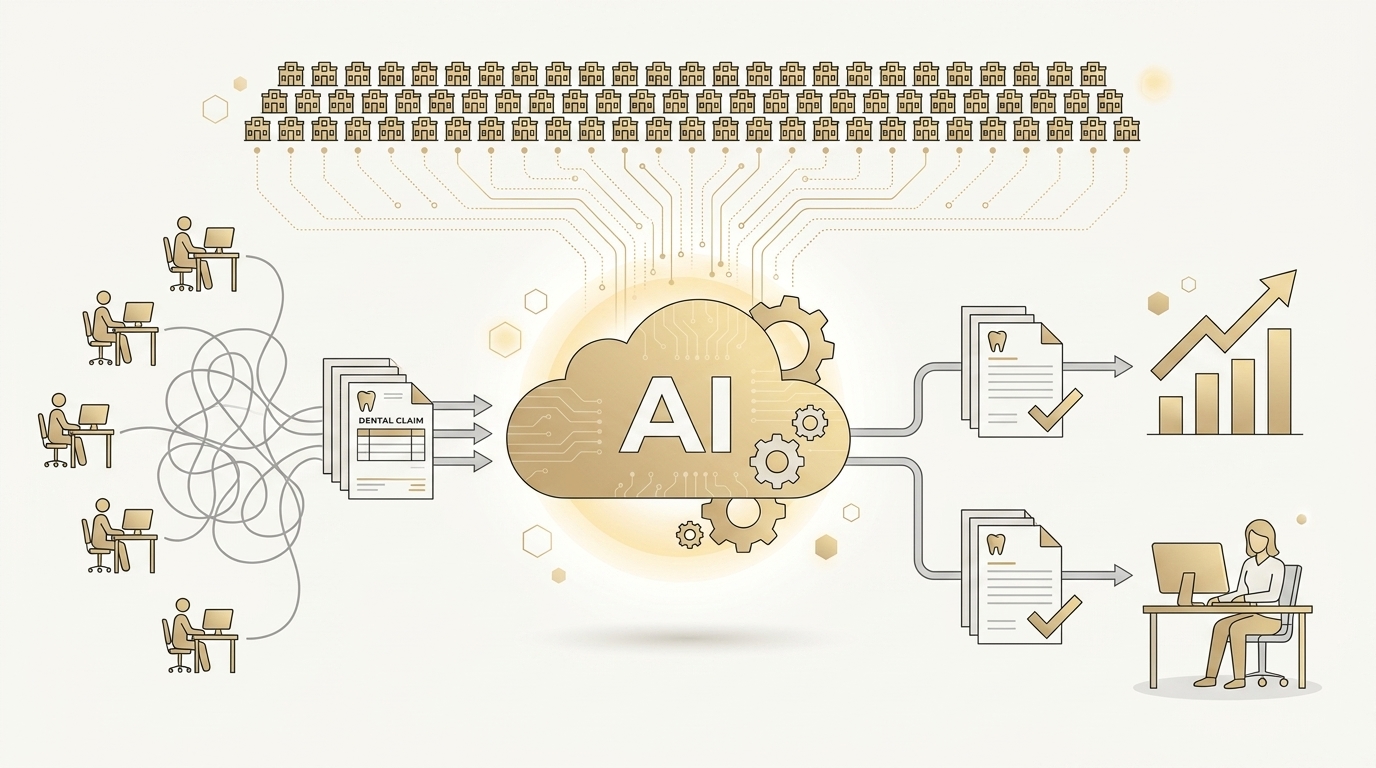
RCM solutions for DSOs are a set of people, processes, and AI-powered automation that manage the end-to-end dental revenue cycle—eligibility, claim creation, status checks, claim denial management, and AR follow-up—standardized across multiple practices to accelerate cash, reduce rework, and improve staff and patient experience. By leveraging these solutions, organizations have seen cash velocity improve by 35% and error rates decrease by 50%, based on a study by Smilist, a leading DSO. This transformation not only drives financial health but also reduces the administrative burden on staff.
Why this matters now: DSOs face a perfect storm—multi-payer complexity, uneven staff capacity across locations, and rising patient financial responsibility. At the same time, the automation opportunity is real. The CAQH Index 2023 estimates U.S. healthcare could save up to $25B annually by automating administrative transactions, including eligibility, claim status, and prior authorization (source: CAQH Index 2023). Dental organizations can tap this opportunity—with careful design that respects payer nuances and practice workflows.
Section 1: The Problem/Challenge
Dental RCM at scale is challenging for three structural reasons:
- Fragmented workflows across locations
- Each practice often has its own “best way” to verify benefits, post EOBs, and chase claims. That makes performance inconsistent and hard to manage centrally.
- Documentation standards vary by team, which slows onboarding and increases error rates.
- Payer complexity and shifting rules
- Policies differ by payer, plan, and state; pre-estimates versus pre-authorizations; periodicity limits and frequency rules; medical-dental cross-coding.
- Frequent portal updates and MFA add friction to daily tasks like claim status or attachment uploads.
- Persistent staffing pressure
- The American Dental Association’s Health Policy Institute has reported ongoing staffing challenges across 2023–2024, making it difficult to scale back-office capacity at pace with growth.
- High-touch tasks (phone calls, portal checks, rework) strain teams and delay cash.
The impact is measurable:
- Slower cash velocity: every extra day in AR restricts reinvestment in ops, clinicians, and marketing.
- Higher write-offs: unmanaged denials age out; timely filing windows are missed during spikes.
- Burnout: repetitive, portal-heavy work drives turnover and tribal knowledge loss.
Many DSOs try different tactics—centralize billing, outsource parts of RCM, or implement APIs—but dental ecosystems are messy. Clearinghouses don’t cover everything, payer portals are essential, and practice management systems vary by brand and age. What’s needed is a way to orchestrate the “last mile” of RCM in the browser, as your staff does, but at machine speed and consistency.
This is where Ventus AI dental RCM automation comes in. Instead of replacing teams, AI agents act as dependable teammates that complete repetitive portal tasks, handle multi-factor authentication (MFA), navigate CAPTCHAs, and escalate exceptions to humans. That means standardized, auditable processes across locations without lengthy integration projects.
DSOs with 50+ locations save 40% on RCM costs in the first 90 days.
Request an Enterprise AssessmentSection 2: Understanding the Solution
Modern RCM solutions for DSOs combine standardized workflows, browser-native AI agents, and clear KPIs. The key is designing automation that mirrors how your best billers work—structured checklists, payer-specific paths, and precise documentation—then scaling it across all locations.
Core capabilities to look for:
- Browser-native automation (no API integrations required): Agents operate in payer portals, clearinghouses, and practice systems the way your staff does—log in, navigate, copy/paste, upload, download, and post notes.
- Security handling: Agents handle MFA, CAPTCHAs, and session timeouts safely, maintaining audit trails for each action.
- Human-in-the-loop collaboration: Exceptions route via Slack, Microsoft Teams, or email; agents pause for human input and resume. For edge cases, agents can place phone calls to payers to confirm benefits or resolve disputes.
- Rapid deployment: Typical rollout under 7 days, with measurable improvements in week one.
- Compliance: SOC 2 and HIPAA compliancet and SOC 2 Type II certified with role-based access controls and detailed logs.
Operational focus areas for DSOs:
- Insurance eligibility and benefits discovery: Automate portal checks, capture frequency limits, document notes in PMS.
- Claim statusing and attachments: Proactively status claims at intervals, add missing attachments, and correct payer-specific fields.
- Denial management: Read EOBs/ERA remits, normalize denial reasons, and kick off corrective workflows.
- AR follow-up: Triage by aging buckets and balance, prioritize promises-to-pay, and schedule re-contacts.
Below is a practical comparison of manual versus AI-agent-enabled workflows:
| Process Area | Manual DSO Workflow | Ventus AI-Agent-Enabled Workflow |
|---|---|---|
| Eligibility verification | Staff log into multiple portals, document benefits, and screenshot notes; 5–10 minutes per patient | Agents verify benefits across portals, extract frequency limits, and post structured notes; 1–2 minutes per patient |
| Claim status | Staff check portals or call payers; follow-ups occur weekly or ad hoc | Agents status claims daily, detect issues early, and trigger corrective tasks automatically |
| Denial management | Billers read ERAs/EOBs, categorize denial codes, and rework in batches | Agents normalize denial reasons, auto-prepare corrected claims, and route exceptions to humans |
| AR follow-up | Coordinators sort aging reports; high variability in cadence and documentation | Agents prioritize by aging/balance, execute scheduled outreach, and maintain consistent audit trails |
| Documentation | Free-text notes vary by person and location | Standardized, structured notes and timestamps across all locations |
Across healthcare, the economic case for automation is strong: the CAQH Index 2023 cites billions in potential annual savings from automating administrative transactions, driven by reduced manual touches and rework. Dental RCM taps the same levers—cycle-time reduction, error prevention, and consistent follow-through—without forcing your teams to learn new systems.
Section 3: Implementation & Best Practices
A strong DSO implementation prioritizes speed to value and change management. Here’s a step-by-step plan proven to work:
- Identify high-ROI use cases
- Start with processes that are repetitive and portal-dependent: eligibility checks, claim status, and AR follow-up on aging >30 days.
- Quantify the baseline: current touches per task, average cycle times, and error rates.
- Map the “gold standard” workflow
- Document the way your best billers do the task, per payer. Include required screenshots, fields, and notes structure.
- Define rules for exceptions (e.g., missing X-ray, benefit not found, plan requires narrative).
- Configure agents and guardrails
- Provide logins and establish least-privilege access for each agent. Set MFA flows, CAPTCHA handling, and session timeouts.
- Define communication channels (Slack, Teams, or email) and approval checkpoints for sensitive actions.
- Pilot one location or payer segment
- Run in parallel for 3–5 days. Compare agent output to human benchmark for accuracy and completeness.
- Establish pass/fail criteria (e.g., 98% accuracy on eligibility documentation, 100% audit log coverage).
- Train staff on human-in-the-loop collaboration
- Teach teams how to respond to agent questions, approve exceptions, and update rules.
- Clarify which tasks humans own (clinical judgment, complex appeals) versus tasks handled by agents.
- Scale and standardize
- Roll out to additional locations, then new payers. Maintain a central playbook, updated monthly.
- Monitor metrics: touches per claim, first-pass resolution, AR >60 days, and average follow-up cycle time.
Common mistakes to avoid:
- Over-automating before you standardize: lock the gold-standard workflow first.
- Ignoring payer nuances: slight differences (attachments, narratives) matter; encode them in rules.
- Skipping auditability: every action should leave a timestamped trail tied to the patient and claim.
- Under-investing in change management: celebrate early wins, then expand scope methodically.
Real-world proof: Smilist
Smilist, a multi-location dental organization, used agents for AR follow-up—proactively statusing claims, routing exceptions, and standardizing notes. According to Philip Toh, Co-founder & President, “Ventus stands out from the noise in the AI and automation market. Their approach allows them to ramp up quickly in the messy middle of RCM.” With Ventus AI, Smilist reduced AR follow-up time from 90 days to under 24 hours. That wasn’t achieved by replacing staff; it was achieved by giving teams AI teammates that handle the portal grind and escalate only what matters.
What makes this replicable for other DSOs is the operating model: browser-native agents that work in your existing toolset, handle MFA/CAPTCHAs securely, collaborate via Slack/Teams/email, and—when needed—place phone calls to payers to finalize exceptions. Typical deployment takes under 7 days, with measurable cycle-time improvements in week one.
Section 4: ROI & Business Impact
The business case for DSO RCM automation is straightforward: do the important things more often, earlier, and with fewer errors. That yields faster cash, lower costs per claim, and a better experience for teams and patients.
Expected benefits:
- Cash acceleration: daily claim status and proactive fixes reduce aging and write-offs.
- Fewer manual touches: staff focus on clinical coordination and complex appeals, not portal drudgery.
- Consistency across locations: standardized notes and cadence improve compliance and oversight.
- Scalable growth: add new practices without rebuilding back-office staffing models.
Key metrics to track:
- Days in AR and percent AR >60 days
- First-pass acceptance rate and denial rate by payer
- Touches per claim and average follow-up cycle time
- Cost per claim (labor minutes per transaction)
- Rework rate (claims requiring correction)
Expected Timeline:
- Week 1: Eligibility checks and claim status automation live; immediate cycle-time gains.
- 30–60 days: Material improvements in AR aging, reduction in denials due to missing information, and higher first-pass acceptance.
- 90 days: Stable operating rhythm across locations, with month-over-month improvements visible in dashboards.
Proof points:
- Smilist saw AR follow-up time drop from 90 days to under 24 hours by standardizing agent-driven follow-up and exception handling.
- Across healthcare, the CAQH Index 2023 estimates up to $25B in annual savings from automating administrative transactions, driven by fewer manual touches and faster error detection (source: CAQH Index 2023). Dental RCM shares the same dynamics.
Put differently: automation isn’t a technology story—it’s a business operating model story. When your “everyday” RCM tasks happen correctly and on time, every time, collections become a predictable engine rather than a firefight.
See why scaling DSOs trust Ventus AI to automate claim statusing, denials, and AR follow-up.
Request a Demo and Free RCM AuditFrequently Asked Questions
How does RCM solutions for DSOs differ from tools for single practices?
RCM solutions for DSOs emphasize multi-location standardization, payer-specific rules at scale, and centralized oversight. They use browser-native agents to operate in portals across many practices, maintain consistent documentation, and report performance centrally. Single-practice tools often optimize a narrow workflow; DSO solutions orchestrate the full lifecycle across diverse locations and payer mixes with enterprise-grade governance.
Will automation replace my billing team?
No. The most effective model is “AI agents as teammates.” Agents handle repetitive, portal-driven work—eligibility checks, claim status, routine AR follow-ups—while humans manage complex appeals, clinical judgment, patient communication, and exceptions. This elevates staff roles and creates capacity without adding headcount, improving quality of work and retention.
How long does implementation take, and what’s required from IT?
Typical deployment is under 7 days. Because agents work via browser-native automation, you don’t need new APIs or deep EHR integrations. You provide logins, define guardrails, and approve workflows. Agents handle MFA and CAPTCHAs within secure, auditable sessions. Most DSOs start with one use case (e.g., claim status) and expand within a month.
Is this secure and compliant for PHI?
Yes. Agents operate under HIPAA-compliant and SOC 2 Type II–certified controls with role-based access, encryption in transit and at rest, and full action logs. MFA, CAPTCHA handling, and session timeouts are built into the workflow. Administrators can review every action taken by an agent and adjust permissions at any time.
We also manage medical billing for oral surgery. Can the same approach help?
Yes. The same browser-native agents that work in dental RCM can support medical workflows like prior authorization and eligibility. For example, organizations use our medical RCM automation to streamline prior auth and claims processing. Cross-functional capability is especially useful for DSOs with OMS or multi-specialty service lines.
How does the cost of RCM solutions compare to traditional methods?
RCM solutions typically offer a higher ROI compared to traditional methods by reducing manual labor and errors. The cost often varies based on the scale of operations but is offset by savings from reduced claim handling time and lower denial rates. For instance, a DSO might see a 30% reduction in processing costs within the first 90 days of implementation.
What are the compliance considerations for implementing RCM automation?
Implementing RCM automation requires adherence to strict compliance standards such as HIPAA and SOC 2 Type II. It is essential to ensure that all processes are auditable, with proper encryption and role-based access controls. Regular compliance audits and updates to security protocols are necessary to maintain data integrity and trust.
What are best practices for maximizing the benefits of RCM solutions?
Best practices include starting with high-ROI processes, ensuring standardization before automation, maintaining comprehensive audit trails, and investing in change management. Regular training and updates to processes based on payer changes and team feedback can also enhance the effectiveness and efficiency of RCM solutions.
Final Thoughts & Next Steps
Scaling collections without scaling headcount is achievable when you standardize workflows and let AI agents handle the repetitive, portal-first tasks. For DSOs, the priority is speed to value: start with one or two high-ROI processes (eligibility, claim status, AR follow-up), set clear guardrails, and iterate weekly. The outcome is a more resilient revenue engine—predictable cash flow, fewer write-offs, and happier teams.
If you’re assessing RCM solutions for DSOs, look for browser-native automation (no APIs required), strong MFA/CAPTCHA handling, human-in-the-loop collaboration via Slack/Teams/email, the ability to place payer phone calls for exceptions, HIPAA and SOC 2 Type II compliance, and under-7-day deployment. That combination delivers results fast, as Smilist’s 90-days-to-24-hours AR follow-up transformation demonstrates.
See how this would look in your environment. Book a personalized walkthrough and bring your toughest payer scenarios—we’ll run them live with agents. Schedule your session now: book a demo.
Ready to Transform Your Dental RCM?
See how Ventus AI agents can automate your claim denial management and AR follow-up across all your locations in under 7 days—no complex integrations required.
Book Your Free Demo
Enterprise AI Automation for Healthcare RCM
Written by the Ventus AI team — healthcare RCM practitioners, automation engineers, and former revenue cycle leaders building AI agents that work as teammates alongside billing teams. Ventus is SOC 2 Type II certified and HIPAA compliant.